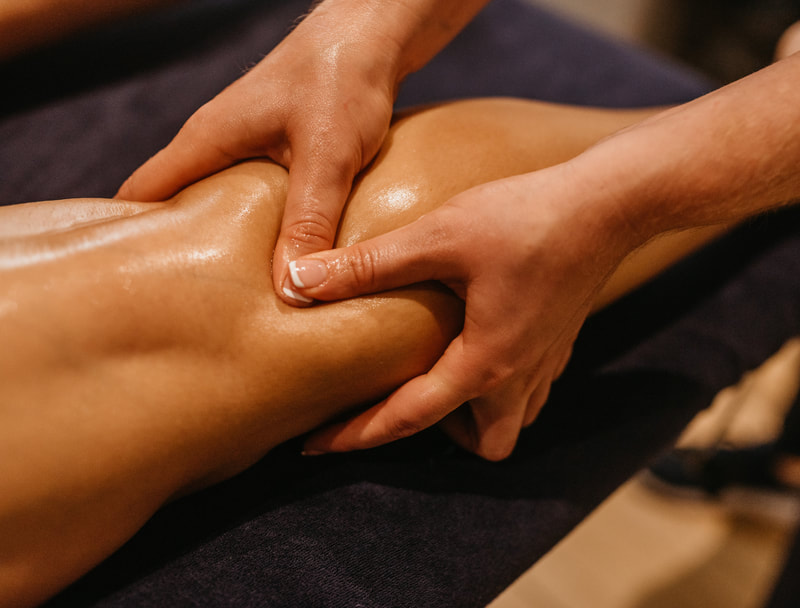
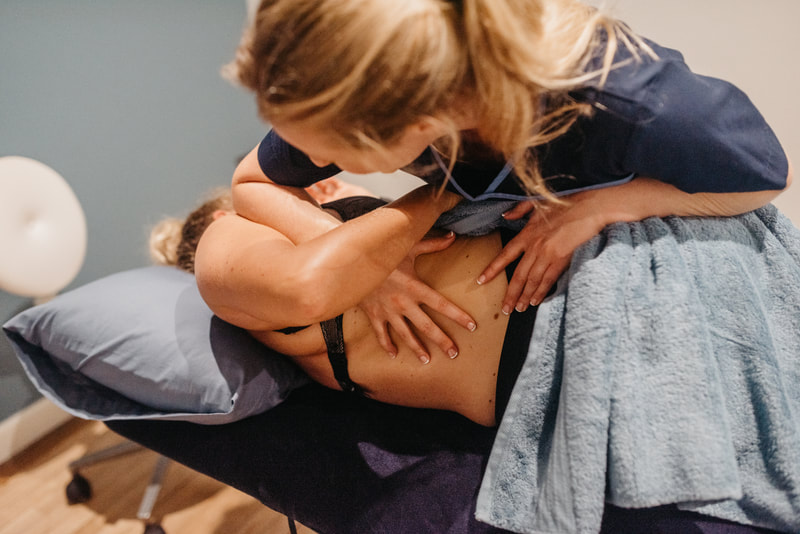
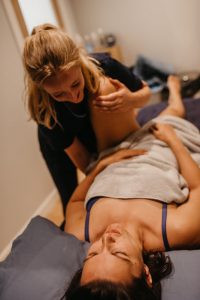
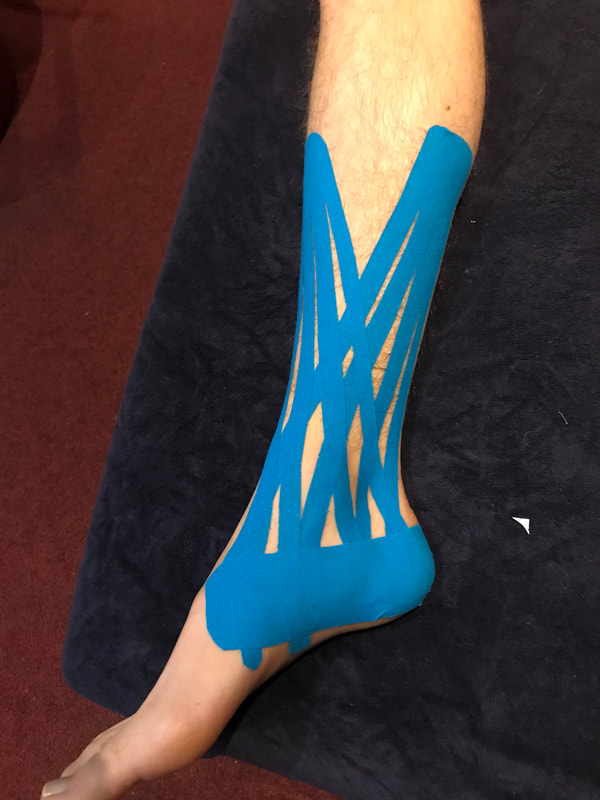
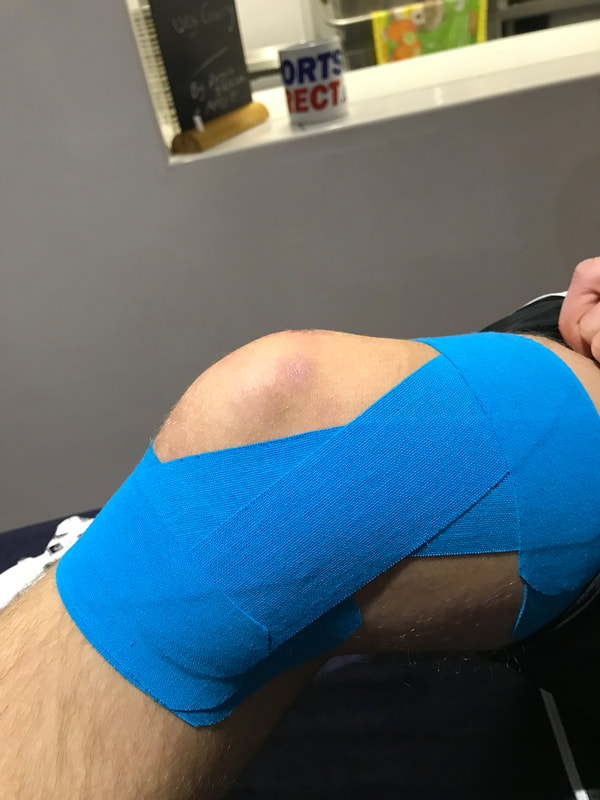
What happens when you visit an Osteopath?
What is a treatment is likely to cost? and How to find an Osteopath near you.
Before you book your first appointment, do call and speak to the receptionist or the Osteopath you would like to see.
Osteopathic practices should be able to provide information about the Osteopath, the clinic, what the treatment involves, payment methods and anything else you need to know in advance of your first visit.
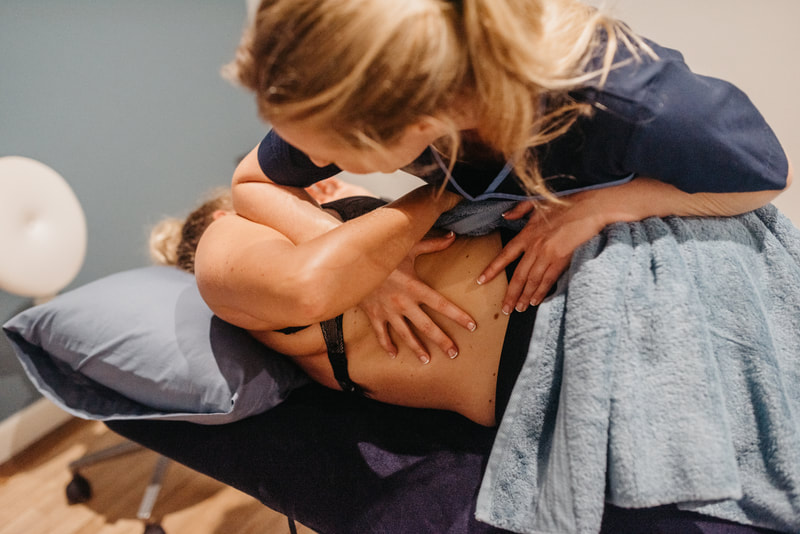
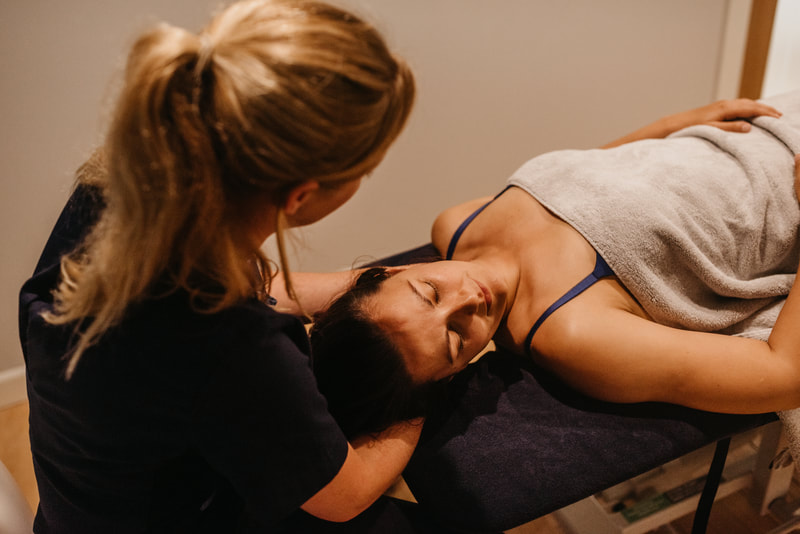
At your first appointment your Osteopath will start by listening to you and assessing you.
Osteopathy is a patient-centred, system of healthcare. A first appointment generally lasts about 45 minutes to allow the osteopath adequate time to:
- Listen and ask questions about your problem, your general health, other medical care you are receiving or medication you are taking, and record this in your case notes. The information you provide will be confidential.
- Examine you properly. It is likely the osteopath will ask you to remove some of your clothing. Tell your osteopath if you are uncomfortable about this. You should expect privacy to undress and a gown or towel should be provided. You can ask a friend or relative to accompany you and be present throughout your treatment.
- Ask you to make simple movements and stretches to observe your posture and mobility. Because of the body’s structure, pain or stiffness you are experiencing in one part may be linked to a problem elsewhere.
- Examine the health of the joints, tissues and ligaments using their hands and a highly developed sense of touch called palpation.
Your osteopath will also check for signs of serious conditions they cannot treat and may advise you to see your GP or go to hospital. They should provide you with a letter explaining what they believe to be the problem.
Diagnosis and treatment
Osteopathy specialises in the diagnosis, management, treatment and prevention of musculoskeletal and other related disorders.
Your osteopath will give you a clear explanation of what they find (their diagnosis) and discuss a treatment plan that is suitable for you. They will explain the benefits and any risks of the treatment they are recommending. It is important to understand and agree what the treatment can achieve, and the likely number of sessions needed for a noticeable improvement in how you feel.
Treatment is hands-on and involves skilled manipulation of the spine and joints, and massage of soft tissues. Your osteopath will explain what they are doing and will always ask your permission to treat you (known as consent). Ask questions at any time if you are unsure what you have been told or if you have any concerns.
Self-help measures and advice on exercise may be offered to assist your recovery, prevent recurrence or worsening of symptoms.
How much does it cost?
Most osteopaths work in the private sector and this means you will usually need to pay for treatment. Fees vary across the UK depending on a number of factors including the osteopath’s location; but the majority of osteopaths tend to charge an initial consultation fee of £55 to £70 and between £40 and £55 for subsequent sessions.
The initial session is often a longer one and generally can last about 45 minutes, with follow-up sessions generally lasting around 30 minutes. But again this will vary.
Most major private health insurance providers provide cover for osteopathic treatment but you will need to ask your insurance company about the level of cover available and whether you need to be referred for treatment first by your GP or a specialist.
Some osteopathic treatment is available through the NHS. For information on who to contact in your region of the UK, ask your GP.
Ongoing care
Because of the physical nature of the treatment, it is not unusual to sometimes feel sore in the first 24-48 hours after treatment. Your osteopath will explain any likely reactions that you could expect. If you have any concerns it is important to contact the osteopath and ask their advice. It may require more than one visit before your problem is resolved. The osteopath will review your progress at each subsequent visit and seek your consent to any changes to your treatment plan.
Is referral from a doctor necessary?
Most patients ‘self-refer’ to an osteopath for treatment, there is no need for a GP letter. You can use the statutory Register of osteopaths on Institute of Osteopathy website to find local osteopaths or simply do an online search.
Although referral by a GP is not necessary, you are encouraged to keep your GP fully informed, so that your medical records are current and complete. This will ensure you receive the best possible care from both health professionals. With your permission, your osteopath may send a report to your GP with details of your condition and treatment. You can also request a letter for your employer if this is helpful.