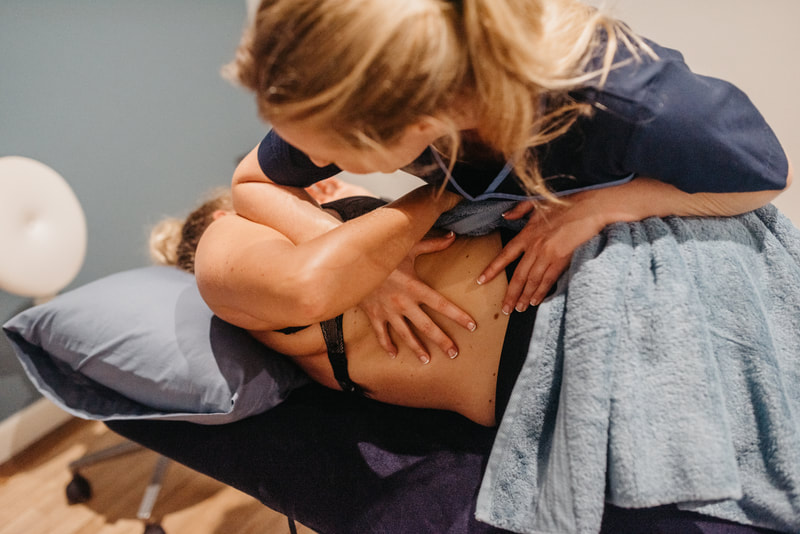
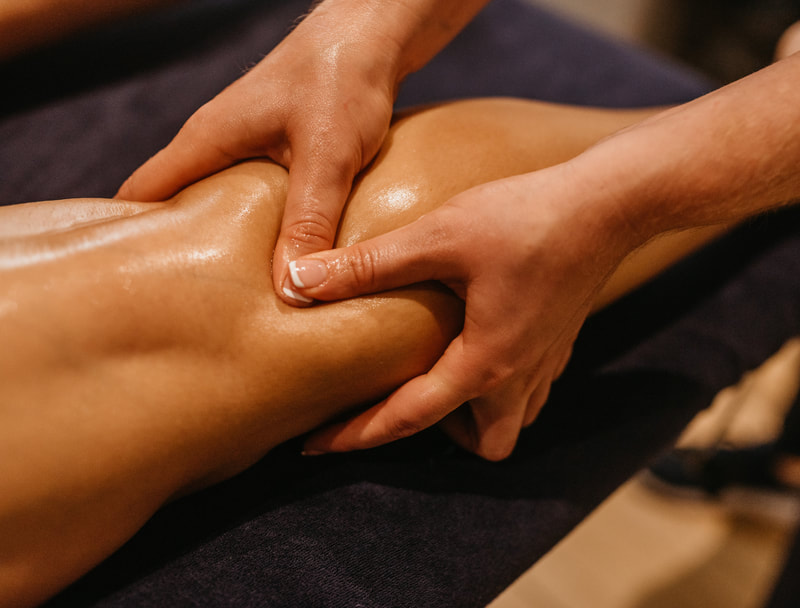
What to expect.
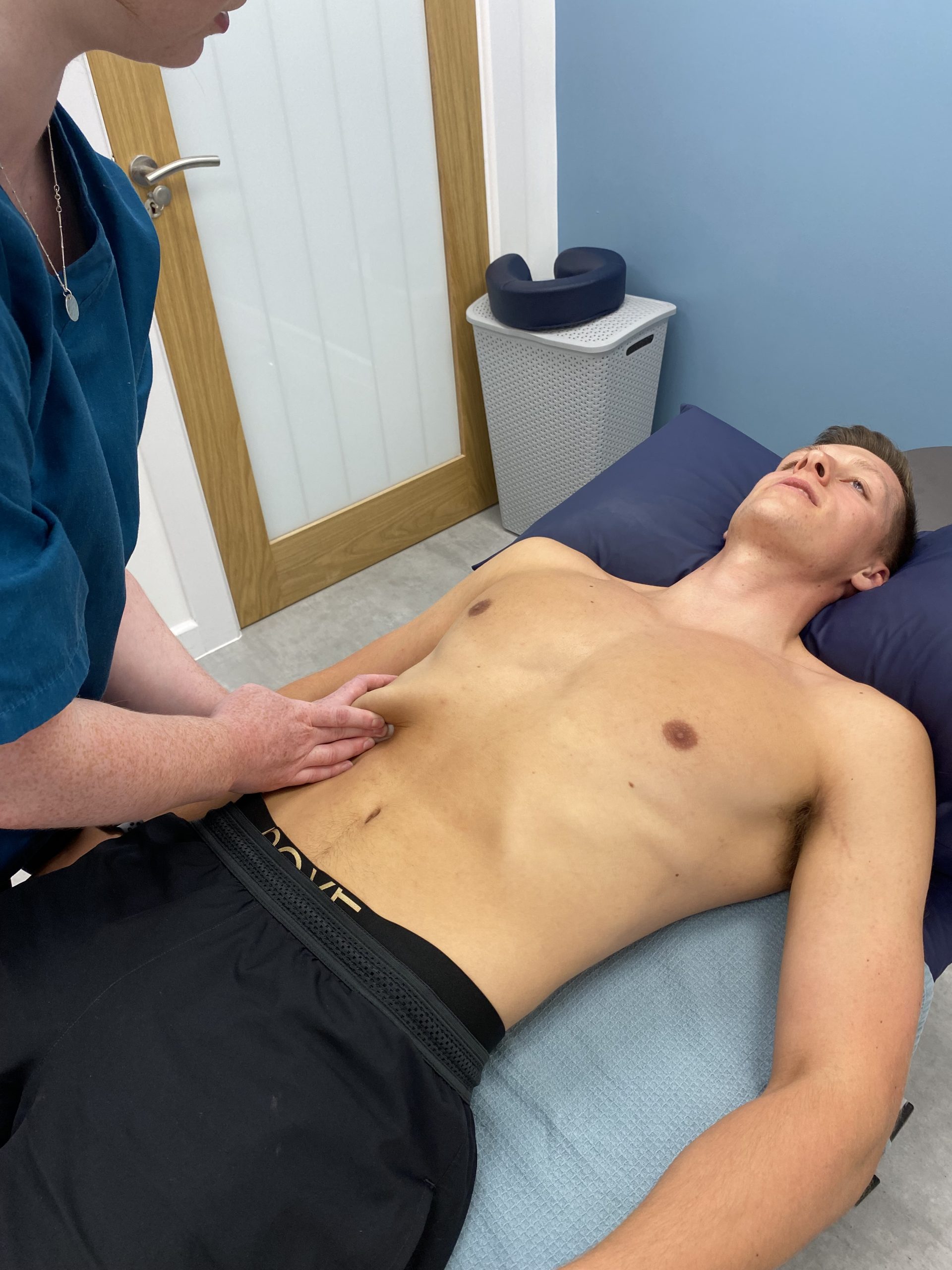
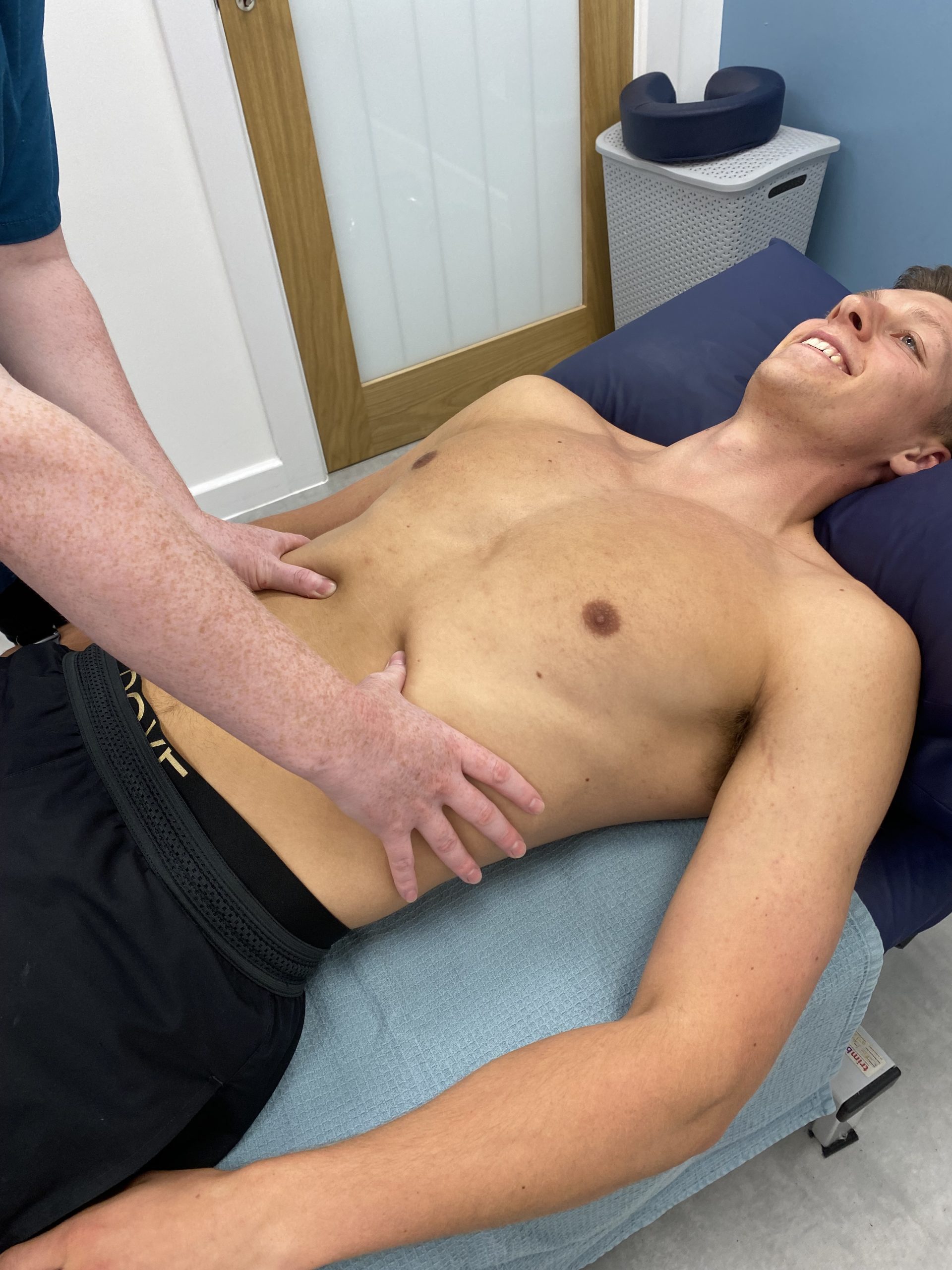
To begin with your practitioner will take a detailed case history of your presenting symptoms, your medical history and some questions surrounding your pregnancy and what you are looking to achieve from the treatment. We will then run though an examination of the area where you are experiencing pain and any global postural patterns.
Treatment usually consists of massage mobilisation and sometimes where appropriate manipulation.
Keeping you and your bump safe and comfortable
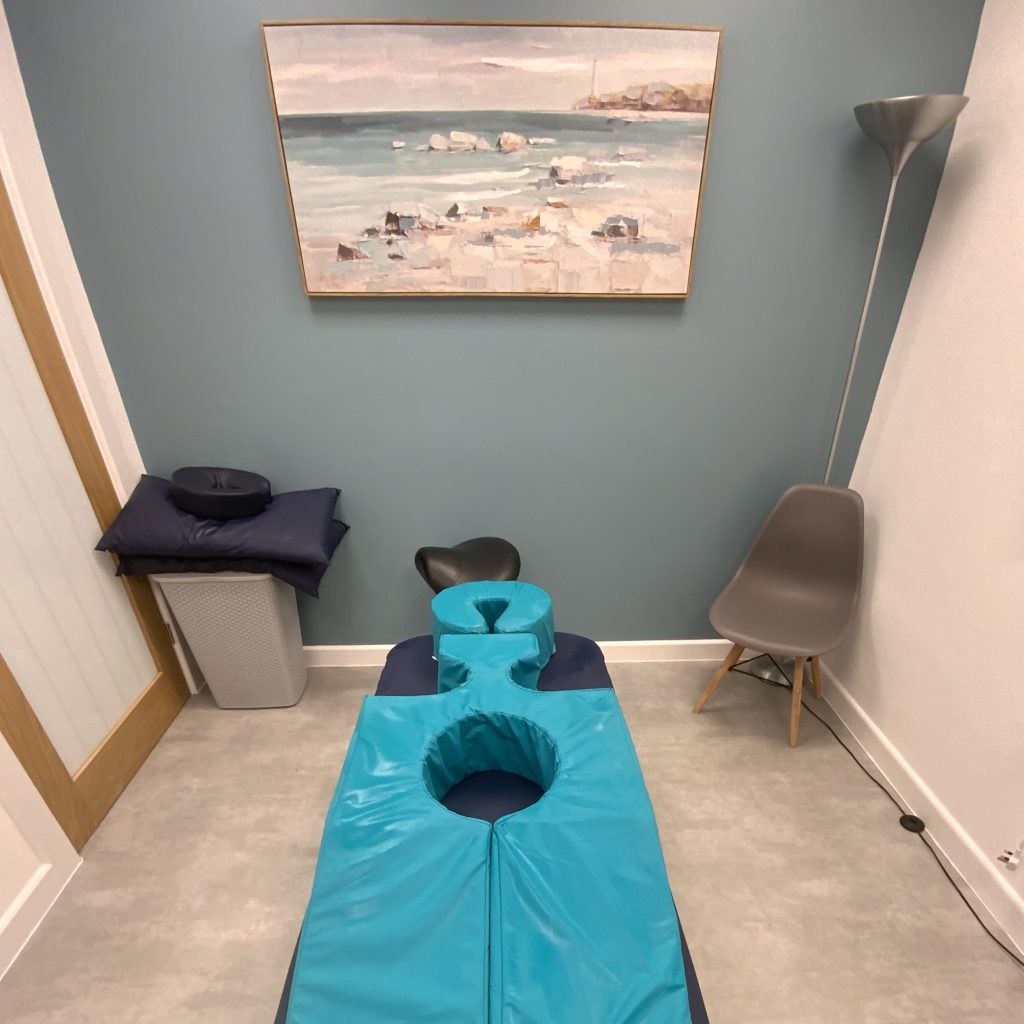
Pregnancy Pillow
Our aim is to keep you and your baby as comfortable as possible whilst we deliver our treatment. We often will use a pregnancy pillow, this can be seen in the photograph to the right. We make sure you are supported on your front and that your bump is not being restricted in any way or touching the couch below. This can be a very comfortable position to receive treatment.

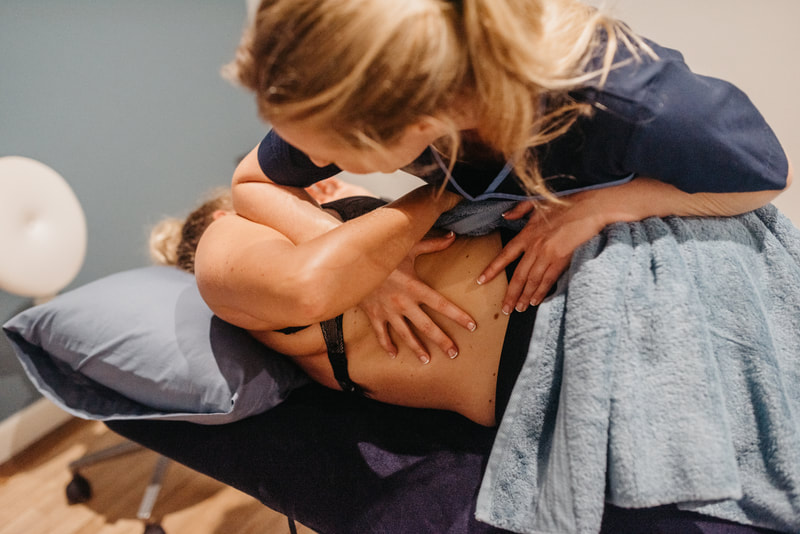
Side laying
Side laying is more useful for some Osteopathic techniques as it allows the body to move in away that just isn’t achievable when you are lying prone. We use pillows placed between your knees and under your bump to make sure you are supported and comfortable.
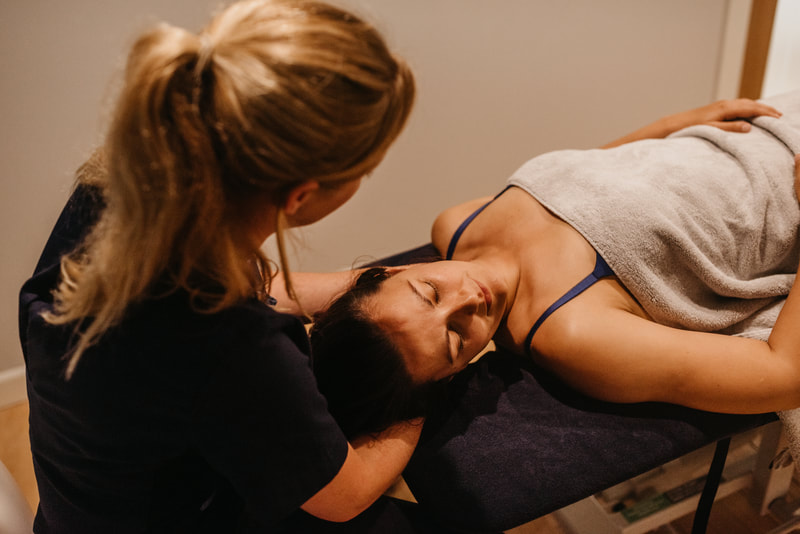
Sometimes we will work with you laying on your back especially when working on your neck and shoulders but the couch is usually propped up at around 45 degrees and we check regularly to make sure you are feeling well and comfortable throughout the session, however if this isn’t working for you most of these techniques can be done in a seated position too.
Treatment is always adapted for you as an individual and we plan our treatment techniques to suit you and your pain presentation. This being said, if you would specifically like massage techniques using the pregnancy pillow please let your practitioner know and we will use it providing it is safe and comfortable to do so.